1. What is HPV?
Human papillomavirus (HPV) is one of the most common groups of viruses worldwide. Most people will have an HPV infection at some point in their lives, but in most cases, it goes away on its own.
2. What are the signs and symptoms of HPV?
HPV can affect anyone, regardless of gender. Most people with HPV don’t experience symptoms and may not even know they are infected.
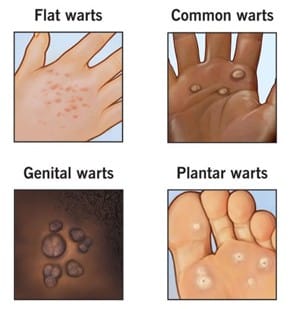
Low-risk types of HPV can cause warts, which may appear as small skin tags on the hands, feet, or genitals. These warts can be itchy or uncomfortable but are not dangerous.
High-risk types of HPV often remain unnoticed until they lead to serious health issues, such as cancers of the cervix, vagina, vulva, anus, penis, or the back of the throat (known as oropharyngeal cancer). Read Cervical Cancer Facts
3. How is HPV spread?
HPV infection happens when the virus enters the body, often through small cuts or breaks in the skin. The virus spreads mainly through skin-to-skin contact.
Genital HPV spreads through:
- Vaginal, oral and anal sex with an infected partner.
- Skin-to-genital contact, even without penetration.
4. How do you test for HPV?
HPV testing is usually part of cervical cancer screening for women. The most common tests are:
- HPV DNA test: Detects high-risk types of HPV that can lead to cancer.
- Pap smear: Looks for abnormal cervical cells that may be caused by HPV.
Currently, there is no routine HPV test for men. However, regular check-ups and being aware of any symptoms are important.
5. How to protect yourself against HPV?
While you can’t eliminate the risk of HPV, there are effective ways to lower your chances of infection and prevent complications. Instead, focus on practical steps that reduce the risk of infection and help protect your health while maintaining a healthy sex life. You can reduce your risk by:
- Get vaccinated against HPV: The HPV vaccine protects against the most common types of the virus that can cause cancer and warts.
- Go for regular cervical screening.
6. What are the treatment options for HPV?
There is currently no cure for HPV itself. Most HPV infections do not cause any issues and are cleared naturally by your immune system within 2 to 3 years. However, treatments are available for health problems caused by HPV, such as genital warts, cervical precancers, and cervical cancer.
If a high-risk HPV infection is detected, your doctor may recommend a closer examination of your cervix using a special microscope. This is called a colposcopy, and it helps check for any signs of precancer or cancer. Learn more about what happens after your HPV test in our Follow-Up Care section.
Common Myths and Misconceptions about HPV
Myth: Only people with multiple partners get HPV.
Fact: Anyone who has ever been sexually active can get HPV, even with just one partner.
Myth: HPV infection will always cause cancer.
Fact: Most HPV infections do not cause cancer. However, almost all cases of cervical cancer are linked to HPV.
Myth: If a woman’s mother or grandmother had cervical cancer, she will get it too.
Fact: Most types of cervical cancer are not hereditary.
Myth: HPV vaccination protects against all strains of HPV.
Fact: The HPV vaccine protects against the most common cancer-causing types, but not all HPV strains.
Myth: Vaccinated women no longer need cervical screening.
Fact: Women still need regular screening. A combination of HPV vaccination and cervical screening gives the best protection.
Myth: HPV vaccination can affect a girl’s fertility later in life.
Fact: The HPV vaccine is safe and does not affect future fertility.
Myth: Using a condom completely protects against HPV.
Fact: Condoms reduce the risk but do not provide full protection against HPV.
Myth: Women who have not been sexually active for a long time have no risk of cervical cancer.
Fact: Cervical cancer can take 10–20 years to develop, so regular screening remains important even for women who are not currently sexually active.
Myth: Antibiotics can treat HPV infection.
Fact: HPV is a viral infection. Antibiotics are not effective against viruses.
Myth: HPV can be caught from sharing clothes or toilet seats.
Fact: HPV spreads through skin-to-skin or skin-to-genital contact, not through clothes or toilet seats.
Myth: HPV is a sexually transmitted disease (STD).
Fact: HPV is a very common infection that is typically spread through sexual contact, but it is often different from traditional STDs like gonorrhea or chlamydia.
Myth: Contact tracing is needed if a woman tests positive for high-risk HPV.
Fact: Contact tracing is not necessary for HPV, because it is not considered a traditional sexually transmitted disease.
